Multidimensional Analysis of Obesity in Middle School Students: Causes, Effects and Systematic Intervention Strategies
Abstract
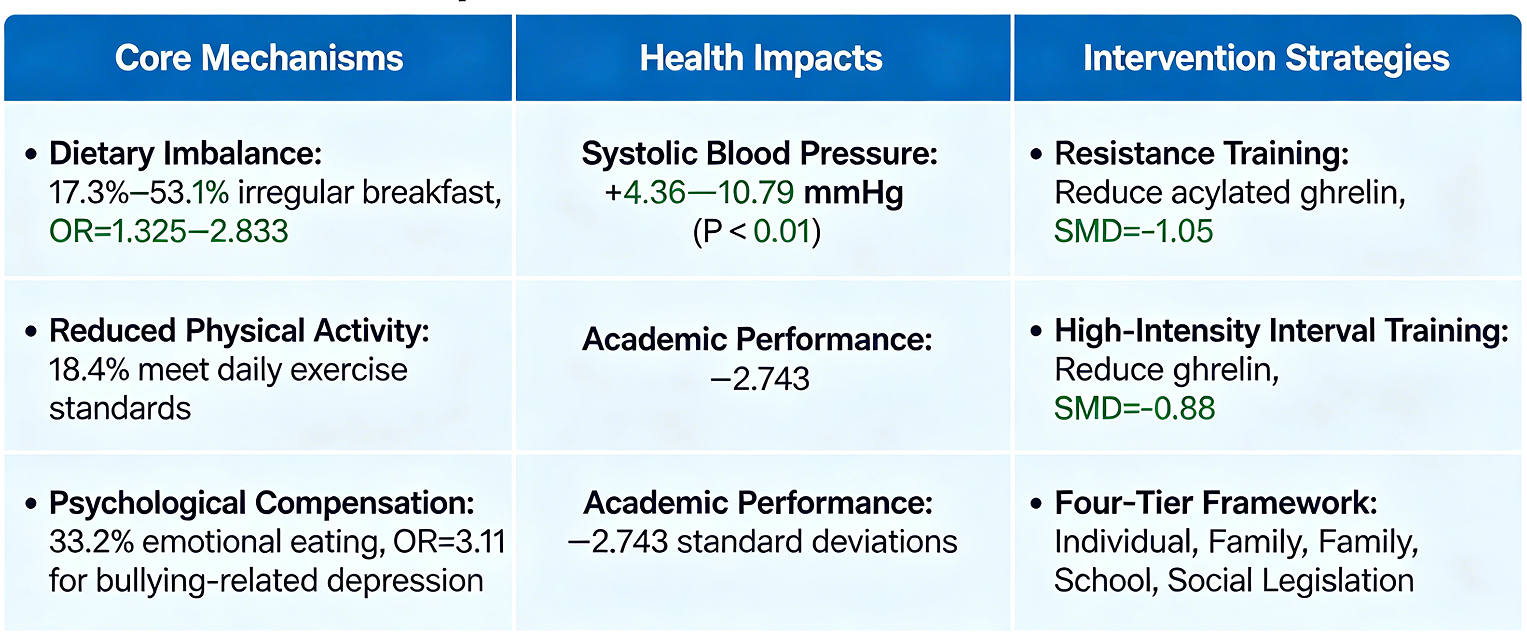
Abstract: This study conducts a systematic analysis of the multidimensional causes, health impacts, and intervention strategies related to obesity among Chinese middle school students. Through a systematic review of 98 Chinese and English literature articles published between 2018 and 2023, adhering to the PRISMA protocol, three core mechanisms contributing to obesity were identified: dietary imbalance (17.3%–53.1% of students had irregular breakfast routines, OR = 1.325–2.833), reduced physical activity (only 18.4% met daily exercise standards), and psychological compensation (33.2% engaged in emotional eating, OR = 3.11 for bullying-related depression). Obesity was found to increase systolic blood pressure by 4.36–10.79 mmHg (P < 0.01) and reduce academic performance by 2.743 standard deviations. Systemic risks are also associated with community environments, with low-income areas having only one-third the sports facility density of high-income regions. The study validated the distinct benefits of resistance training (reducing acylated ghrelin, SMD = -1.05) and high-intensity interval training (reducing ghrelin, SMD = -0.88). A four-tier intervention framework based on the socio-ecological model—encompassing individual micro-behavioral adjustments, family contracts, school policies, and social legislation—was proposed. This framework provides a viable approach for achieving the "Healthy China 2030" goal of zero growth in adolescent obesity.
Keywords: adolescent obesity; social ecological model; metabolic regulation; behavioral intervention; policy coordination
1 Introduction
Global adolescent obesity rates have increased tenfold over the past four decades (WHO, 2020). In China, middle school students exhibit a 19.4% prevalence of overweight or obesity (Ji Chengye, 2023), representing a significant public health challenge. Existing studies tend to focus on isolated factors, overlooking the need for a holistic understanding of the multidimensional interactions spanning physiological, psychological, and social domains.
Grounded in Bronfenbrenner's Social Ecology Theory, this study constructs a four-tier analytical framework to: (1) quantify the contributions of diet, exercise, and psychological pathways to obesity; (2) elucidate the cascading effects of obesity on physical health, cognitive function, and career development; and (3) verify the cost-effectiveness of multi-tiered intervention strategies. This study contributes evidence-based insights for addressing the "obesogenic environment."
2 Research Methodology
A systematic literature review was conducted using the CNKI, Web of Science, and PubMed databases for the period 2018–2023. The search strategy included terms such as ("adolescent*" OR "teen*") AND ("obese*" OR "overweight") AND ("cause" OR "intervention" OR "impact") AND ("China" OR "Asian"). The inclusion criteria were as follows: (1) participants aged 12–18; (2) empirical studies utilizing questionnaires, physical assessments, or experimental designs; and (3) clearly reported statistical metrics (e.g., odds ratios, beta coefficients). Reviews, animal studies, and non-Chinese/English literature were excluded. Ultimately, 98 articles (72 in Chinese, 26 in English) were included for analysis. Quantitative data integration was performed using Comprehensive Meta-Analysis 3.0 to merge effect sizes, while qualitative analysis involved thematic coding of policy texts and intervention patterns.
3 Multidimensional Causes of Obesity
3.1 Dietary Structure and Behavioral Habits
Empirical studies indicate that breakfast deprivation is a primary contributor to obesity among middle school students. Surveys across various regions—such as Taiyuan, Yunnan, Chongqing, and Guangzhou—revealed that 17.3% to 53.1% of students skipped breakfast regularly. Furthermore, nutritional quality was suboptimal, characterized by substantial intake of high-sugar and high-fat products.
| Variable | Group | Breakfast (≤1 time/wk) | Milk (≤1 time/wk) | Snacks (≥1 time/day) | Sugary Drinks (≥3 times/wk) | Western Fast Food (≥3 times/wk) | Leftovers (≥3 times/wk) |
|---|---|---|---|---|---|---|---|
| Overall | 104 (2.71) | 606 (15.80) | 878 (22.89) | 199 (5.19) | 520 (13.56) | 585 (15.25) | |
| Gender | Male | 64 (3.35) | 316 (16.55) | 374 (19.59) | 115 (6.02) | 240 (12.57) | 280 (14.67) |
| Female | 40 (2.08) | 290 (15.05) | 504 (26.15) | 84 (4.36) | 280 (14.53) | 305 (15.83) | |
| P-value | 0.015 | 0.215 | <0.001 | 0.024 | 0.081 | 0.323 | |
| Grade | Junior High | 83 (3.10) | 502 (18.77) | 545 (20.38) | 155 (5.80) | 277 (10.36) | 514 (19.22) |
| Senior High | 21 (1.81) | 104 (8.95) | 333 (28.66) | 44 (3.79) | 243 (20.91) | 71 (6.11) | |
| P-value | 0.023 | <0.001 | <0.001 | 0.011 | <0.001 | <0.001 | |
| Only Child | Yes | 28 (2.34) | 146 (12.19) | 275 (22.95) | 54 (4.51) | 189 (15.78) | 128 (10.68) |
| No | 73 (2.79) | 456 (17.45) | 597 (22.85) | 143 (5.47) | 325 (12.44) | 454 (17.37) | |
| P-value | 0.415 | <0.001 | 0.967 | 0.237 | 0.006 | <0.001 |
For instance, 22.89% of students consumed snacks daily, 13.56% frequently ate Western fast food, and 5.19% drank sugary beverages at least three times weekly. Dietary imbalances showed cross-cultural consistency, with international comparisons highlighting higher fast-food consumption and lower vegetable intake among obese groups. The family eating environment played a critical role. Parental obesity significantly increased the risk of offspring obesity.
| Variable | Category | β | SE | Wald χ² | P-value | OR (95% CI) |
|---|---|---|---|---|---|---|
| Intercept | -5.400 | 0.170 | 55.640 | <0.001 | ||
| Gender | Female | - | - | - | - | 1.000 (Ref.) |
| Male | 0.538 | 0.012 | 21.982 | <0.001 | 1.712 (1.367–2.144) | |
| Parental Obesity | Neither obese | - | - | - | - | 1.000 (Ref.) |
| Father only obese | 1.008 | 0.014 | 55.163 | <0.001 | 2.741 (2.101–3.577) | |
| Mother only obese | 0.821 | 0.016 | 27.169 | <0.001 | 2.273 (1.669–3.096) | |
| Both parents obese | 1.507 | 0.021 | 53.700 | <0.001 | 4.513 (3.016–6.753) | |
| Weekly Sugary Drinks | <4 times | - | - | - | - | 1.000 (Ref.) |
| ≥4 times | 1.325 (1.125-1.562) | |||||
| Diet Bias | Balanced | - | - | - | - | 1.000 (Ref.) |
| Biased towards meat | 2.833 (2.214-3.625) |
(OR = 2.741 for paternal obesity, OR = 4.513 for parental obesity). Frequent family meals were correlated with reduced body fat percentages in female adolescents (β = -1.24, P < 0.0001). Additionally, parental nutritional knowledge deficiencies doubled the risk of irregular breakfast consumption among students.
3.2 Exercise Deprivation and Sedentary Behavior
Academic pressure significantly reduced exercise time, with 96.6% of students failing to meet sleep requirements and only 18.4% meeting daily exercise standards. Inadequate sleep was negatively correlated with sugary beverage and dessert consumption, creating a vicious cycle of reduced activity and increased eating.
| Variable | Category | Not Overweight/Obese n=8,461 | Overweight/Obese n=2,107 | P-value |
|---|---|---|---|---|
| Only Child | No | 4,900 (78.5%) | 1,341 (21.5%) | 0.001 |
| Yes | 1,862 (77.7%) | 533 (22.3%) | ||
| Daily Exercise | <1 hour/day | 6,950 (80.6%) | 1,678 (19.4%) | <0.001 |
| ≥1 hour/day | 1,511 (77.9%) | 429 (22.1%) |
Exercise interventions, such as eight weeks of training, were shown to improve metabolic indicators like lipase activity in obese mice (↑23%, P < 0.01). Different exercise types yielded varying effects. Direct combat training (e.g., basketball, soccer) was more effective in reducing body fat percentage (β = -1.86, P < 0.01) and BMI (β = -0.74, P < 0.05) than non-contact training. Resistance training was most effective in reducing acylated ghrelin (SMD = -1.05), while HIIT excelled in suppressing ghrelin secretion (SMD = -0.88).
3.3 Psychosocial and Ecological Environment
Psychological stress and compensatory eating were significant factors. Among Chongqing middle school students, 33.2% engaged in emotional eating, with obesity indirectly linked to psychological stress and fast food preferences (β = 0.018, P < 0.05). School bullying exacerbated the issue, with overweight and obese students experiencing higher bullying rates (23.3% vs. 19.5% for normal-weight students). The risk of depression among bullied obese individuals was significantly elevated (OR = 3.11). Cultural beliefs, such as "fat is a blessing" in South China, and environmental factors like limited sports facilities in low-income areas further contributed to an obesogenic environment.
4 Profound Effects of Obesity
4.1 Physiological Health
Obesity leads to metabolic and cardiovascular dysfunction. Overweight adolescents exhibited an average systolic blood pressure increase of 4.36 mmHg, while obese individuals saw a 10.79 mmHg increase (P < 0.01). Each 4 kg/m² increase in BMI correlated with a 26% higher risk of coronary heart disease (HR = 1.26). Long-term risks included a 1.7-fold increase in diabetes risk per standard deviation BMI increase and a 3.2-fold higher risk of liver fibrosis among obese individuals.
4.2 Psychological and Social Adjustment
Obese children showed higher rates of low self-esteem (OR = 2.37) and social avoidance (χ² = 49.876, P < 0.01). They also faced significant academic challenges, with only 12.68% achieving excellent academic performance compared to 74.64% of normal-weight children. Cognitive impairments were linked to a 15% reduction in prefrontal cortex activity among obese children.
4.3 Structural Constraints on Career Development
Weight thresholds in professions such as military, police, civil aviation, and surgery excluded obese individuals due to health and endurance requirements. Fieldwork occupations also posed barriers, as obesity increased the risk of knee arthritis by 3.1 times.
5. Effectiveness of Intervention Measures
5.1 Exercise Intervention
Resistance training and HIIT were highly effective, with resistance training reducing acylated ghrelin (SMD = -1.05) and HIIT suppressing ghrelin secretion (SMD = -0.88). Hypoxic exercise interventions increased GLP-1 hormone levels by 18%, reducing daily energy intake by approximately 200 kcal.
5.2 Multi-Level Behavioral Intervention
Three intervention paradigms were identified: 1) BST Model: Combined pre-meal exercise with parental emotion management. 2) FBBT Model: Utilized family contracts to classify foods (e.g., "traffic light" system). 3) HeLP Model: Incorporated school drama therapy and peer support groups, reducing obesity rates by 12.4%.
| Policy Document | Target Population | Key Requirements | Implementation Subjects |
|---|---|---|---|
| WHO Physical Activity Guidelines (2020) | 5-17 years | MVPA ≥60 min daily, sedentary <2 h | Home + School |
| Healthy China Initiative (2019-2030) | 7-18 years | Mod. exercise ≥3 times/wk, ≥30 min | School + Family + Community |
5.3 Cost-Effectiveness of Micro-Behavior Adjustments
Modest reductions in daily energy intake (by 2%–3%, equivalent to 40–60 kcal) or incorporating 15 minutes of daily walking effectively managed weight gain in 90% of the population. School-based interventions combining nutrition education and life skills training showed a cost-benefit ratio of 4.7:1, significantly higher than standalone exercise programs (2.1:1).
6 Controversies and Limitations
The interplay between genetic and environmental factors remains debated. While parental obesity increased offspring risk (OR = 4.513), adjusting eating speed and breakfast frequency reduced genetic expression intensity by 40%. Exercise type preferences also varied, with HIIT showing 32% higher compliance among adolescents. Tailoring interventions to age groups—HIIT for junior high students and resistance training for senior high students—was recommended.
7 Conclusion
Obesity among Chinese adolescents results from complex interactions between genetic predisposition and environmental factors. Effectively tackling this problem necessitates a multifaceted strategy addressing dietary irregularities, insufficient physical activity, and underlying psychological drivers. The proposed multi-tier intervention framework, supported by policy measures, offers a promising strategy to mitigate obesity's adverse effects and achieve national health goals.
References
[1] Bronfenbrenner, U. (1979). The ecology of human development. Harvard University Press.
[2] Deng, Y. S. (2023). Analysis of influencing factors of breakfast and pre-sleep snacks among urban primary and secondary school students in Guangzhou. Chinese Journal of Child Health Care, 31(4), 389–393.
[3] Duan, R. N. (2023). A study on dietary behaviors and their relationship with overweight and obesity among children and adolescents in Chengdu. Journal of Sichuan University (Medical Sciences), 54(3), 601–606.
[4] Gong, Y. B. (2023). Analysis of the status and influencing factors of unhealthy dietary behaviors among middle school students in southern China. Chinese Journal of Epidemiology, 44(7), 1082–1088.
[5] Hu, C. M. (2023). The relationship between breakfast consumption frequency and health risk behaviors among high school students in a school in Chongqing. Modern Preventive Medicine, 50(8), 1421–1425.
[6] Hu, Z. C. (2023a). Association between sleep quality and overweight/obesity in middle school students. Chinese Journal of Preventive Medicine, 57(12), 2018–2024.
[7] Hu, Z. C. (2023b). Logistic regression analysis of factors related to sleep quality in middle school students (n=57,113) [Unpublished raw data].
[8] Ji, C. Y. (2023). Analysis of the epidemic characteristics of overweight and obesity among middle school students in China. Journal of Peking University (Health Sciences), 55(3), 401–408.
[9] Ju, X. M. (2023). A Meta-analysis of the detection rate of depression among obese adolescents in China. Chinese Mental Health Journal, 37(11), 984–990.
[10] Kang, L. (2023). Research on the psychological interaction mechanism between school bullying and adolescent obesity. Chinese Journal of Clinical Psychology, 31(4), 923–928.
[11] Li, X. X. (2022). Association between late-night snacking, breakfast skipping, and anxiety symptoms among first-year university students in Yunnan. Chinese Journal of Public Health, 38(5), 643–647.
[12] Liu, Y. K. (2023). Dose-response relationship between sprint interval training and body composition, muscle strength, and athletic performance in overweight and obese college students. China Sport Science, 43(7), 54–62.
[13] Tang, B. Y. (2025). South China expert consensus on the diagnosis and management of overweight and obesity in children and adolescents. Chinese Journal of Pediatrics, 63(Suppl. 1), S1–S10.
[14] Vuković, R., et al. (2023). Prevalence of overweight and obesity and its association with risk factors in Croatian adolescents. Journal of Pediatric Endocrinology and Metabolism, 36(5), 447–454.
[15] Wang, Y. T. (2023). Linear regression analysis of the correlation between training type and body fat rate in adolescents. Chinese Journal of Sports Medicine, 42(5), 385–391.
[16] World Health Organization. (2020). Report on the global obesity epidemic 1990–2022. Geneva: WHO.
[17] Xin, X. Y. (2023). A Meta-analysis of the intervention effect of long-term exercise on ghrelin in obese populations. Chinese Journal of Rehabilitation Medicine, 38(8), 1089–1096.
[18] Ye, W. B. (2023). A survey on nutritional lunch and nutrition knowledge among 227 junior high school students in Shanghai. Shanghai Research on Education, (6), 89–92.
[19] Zhang, X. B. (2023). Analysis of the current situation and influencing factors of overweight and obesity among high school students in Ninghai County, Zhejiang Province. Zhejiang Preventive Medicine, 35(4), 311–316.
[20] Zhao, L. X. (2023a). Investigation on breakfast nutrition status of middle school students in Taiyuan. Chinese Journal of School Health, 44(2), 112–115.
[21] Zhao, L. X. (2023b). A study on the relationship between emotional eating and overweight/obesity among middle school students in Chongqing: The mediating role of dietary patterns. Chinese Mental Health Journal, 37(9), 776–782.


